Healthcare app development lives at the collision of clinical workflow, data security, regulation, and legacy integrations. Get it wrong and you burn budget and break care delivery.
The global telehealth market is forecast at roughly $455B by 2030 (24.68% CAGR). U.S. digital health funding rebounded to $14.2B in 2025 (+35% YoY), but capital concentrated into fewer winners, so buyers and investors are pricing workflow ROI now. This healthcare app development guide covers what to build, the compliance and integration work that drives feasibility, real budget ranges, and how to launch and iterate without breaking care delivery.
Table of Contents:
- What is a healthcare app?
- Must-have features in healthcare app development
- The 5 steps to build a healthcare app
- How much does it cost to create a healthcare app?
- Best practices and modern capabilities in healthcare app development
- Monetization models of a healthcare application
- How to choose a healthcare app development company
- What makes healthcare app developers different from general mobile developers
- Develop your healthcare app with Topflight
Key Takeaways
- Treat “healthcare app” as a workflow product first (patients, clinicians, admins, and front-desk staff). Your feature list should map to who does what, when, where, and how it breaks today.
- Start with the boring must-haves (auth/roles, consent, audit trails, data storage, integrations) before “AI/next-gen” add-ons. Otherwise you’ll ship a demo that collapses in real care delivery.
- Budget realistically: a credible MVP usually starts around $60,000+, and costs climb fast once you add integrations, compliance hardening, QA depth, and post-launch maintenance.
- Follow a disciplined build sequence (discovery → UX → architecture → development → launch/iteration) and lock scope per phase. Most “runaway” healthcare projects fail in the handoffs.
- Pick partners like you’re hiring a long-term operator. Prioritize healthcare domain proof, security posture, post-launch support, and references that survived an audit.
What is a healthcare app?
A healthcare app is software that supports care delivery. It can capture patient data, help clinicians document and make decisions, coordinate appointment scheduling, or move information between systems like EHR platforms (often via FHIR/HL7).
Healthcare mobile application development sits where clinical workflow, data security, regulation, and legacy integrations meet. HIPAA, GDPR, FDA SaMD, and SOC 2 each apply depending on use.
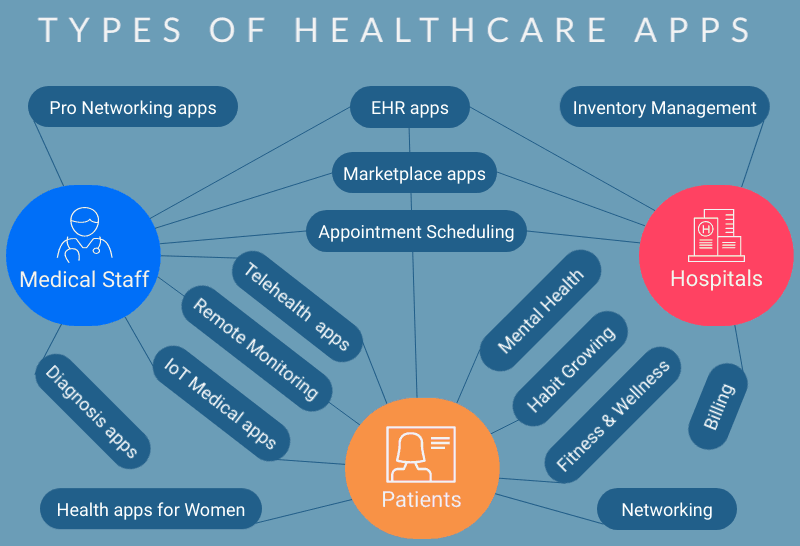
Most teams building a product in medical app development land in one (or more) of these buckets:
- Clinical workflow apps: documentation, clinical decision support, coding support, and order entry
- Patient engagement apps: telemedicine, messaging, education, adherence
- Remote patient monitoring (RPM): wearables, connected medical devices, vitals capture, and alerts
- Care navigation + admin ops: scheduling, intake, benefits, referrals
- Condition-specific digital therapeutics: MSK, mental health, chronic disease programs, and metabolic health
Healthcare apps for providers
Provider apps live inside clinician workflows: documentation, clinical decision support, admin load reduction (burnout’s favorite food), and coding outputs that feed revenue cycle. Abridge and Ambience Healthcare are good examples: they turn patient-clinician conversations into structured documentation and coding outputs that fit real EHR workflows.
Healthcare apps for patients
Patient apps focus on access, adherence, self-management, and engagement. Headspace is a classic patient-facing mental health example (guided sessions + “SOS” moments); PatientsLikeMe shows the community + tracking model for chronic conditions. Conversational interfaces are increasingly common here. If you’re considering how to build a mental health chatbot as part of your patient engagement layer, the technical and compliance requirements differ meaningfully from a general-purpose chatbot.
Health apps for medical administration staff
Admin-facing apps target the operational bottlenecks: appointment booking, intake, insurance/eligibility checks, routing, and patient communications. In many orgs, this is where app development for healthcare quietly pays for itself, because fewer manual handoffs mean fewer no-shows, fewer backlog fires, less staff time on phone tag, and faster intake.
Benefits of healthcare apps for patients
- Faster access to care (telemedicine + scheduling)
- Better continuity (medical history and meds)
- Higher engagement (reminders and patient portals)
- Improved outcomes via monitoring + timely interventions (RPM / wearables)
Benefits of healthcare apps for providers
- Less documentation burden (ambient AI + templates)
- Faster decisions with better data visibility (dashboards and alerts)
- Better coordination across teams (secure messaging + shared plans)
- Cleaner integration into the delivery system (EHR + interoperability)
Must-have features in healthcare app development
If you want healthcare app development to survive real-world care delivery, you need a baseline that covers patient data, HIPAA compliance, data security, and EHR integrations (FHIR/HL7 mapping) before you chase “nice-to-haves.”
Must-have features for patient-facing apps
For many apps, the highest-ROI reminders are medication-related: prescription refills, dose schedules, “missed dose” follow-ups, and titration prompts (with safe defaults and clinician-approved wording). Teams shipping these flows often look for dedicated pharma app development services so refill timing, eligibility checks, pharmacy integrations, and prior-auth handling don’t get bolted on late.
| Feature | Why it matters | Common implementation notes |
|---|---|---|
| Secure sign-up + authentication | Protects access to medical records / sensitive patient data | MFA/2FA, device-based auth, role-aware sessions, and refresh-token rotation |
| Patient profile + medical history | Enables continuity of care and personalization | Structured history, meds, allergies, and immunizations; data validation |
| Appointment booking + scheduling | Direct impact on access + staff workload | Time slots, reminders, cancellation rules, waitlists |
| Telemedicine + secure messaging | Covers remote care + follow-ups (telehealth/telemedicine) | HIPAA-ready video/messaging provider; audit trails |
| Push notifications + reminders | Boosts adherence and reduces no-shows | Medications, appointments, care-plan tasks, and refill reminders |
| Health tracking / RPM inputs | Supports chronic care + monitoring | Wearables (heart rate, blood pressure, glucose levels, weight), manual logs |
| Integrations (HealthKit/Google Fit/Samsung Health/Fitbit) | Faster onboarding + richer health monitoring | Treat as “optional” unless the use case needs it |
| Consent + privacy controls | Regulatory + trust baseline (HIPAA/GDPR) | Granular consent, data export/deletion where applicable |
| Security baseline | Non-negotiable in mobile health app development | Encryption, access controls, audit logging, and key management |
Related: How to Develop a Telehealth App
Related: How to Build a Patient Portal App
Must-have features for provider-facing apps
| Feature | Why it matters | Common implementation notes |
|---|---|---|
| Role-based access control (RBAC) | Keeps protected health information (PHI) scoped to the right medical professionals | Roles like clinician, admin, biller, and front-desk; least privilege |
| Patient search + chart view | Core daily workflow in hospitals/clinics | Fast lookup, filters, “last seen,” active problems |
| Documentation + clinical notes | Reduces admin drag; improves traceability | Templates, voice dictation, structured fields, and autosave |
| Care team collaboration | Smooth handoffs improve patient outcomes | Secure messaging, tasking, escalation paths, and on-call routing |
| EHR integration readiness | Providers won’t retype data forever | APIs, HL7/FHIR mapping, Epic/Cerner constraints, and SMART on FHIR auth |
| Order/referral support (as needed) | Directly supports care delivery operations | LIS, imaging, referrals routing, and pharmacy; permissions baked in |
| Audit logs + reporting dashboards | Compliance + ops visibility | Who accessed what/when, anomaly flags, dashboards, and retention windows |
| Security + compliance controls | Required for clinical environments | Encryption, secure session handling, device policies, and MDM controls |
Also, read our guide on How to Create an EMR/EHR System.
The 5 steps to build a healthcare app
If you’re mapping out how to develop a healthcare app, this healthcare mobile app development guide breaks the development process into five steps that keep delivery grounded in real clinical workflows, patient engagement, compliance, and integration realities (HIPAA, GDPR, FDA SaMD, or SOC 2, depending on scope).
Step #1: Define your audience (discovery & market validation)
Four things to lock down up front: who the primary users are (patients, healthcare providers, admin staff, or some combination), what moment they’re in when they reach for the app (at home, mid-visit, after discharge, between appointments), what “success” looks like in measurable terms (fewer no-shows, faster documentation, lower readmissions, or better patient outcomes), and which assumption is riskiest if you’re wrong. Stakeholder interviews and lightweight market research will surface that before you commit to build a healthcare app.
Add these “context of use” questions before you write a single user story:
- Where will people use the app: at home, in a waiting room, during rounds, between appointments?
- Are they standing, sitting, walking, or juggling two things at once?
- Do they have both hands free, or is this a one-thumb experience?
- Are they using it while talking to a patient (i.e., interruptions are guaranteed)?
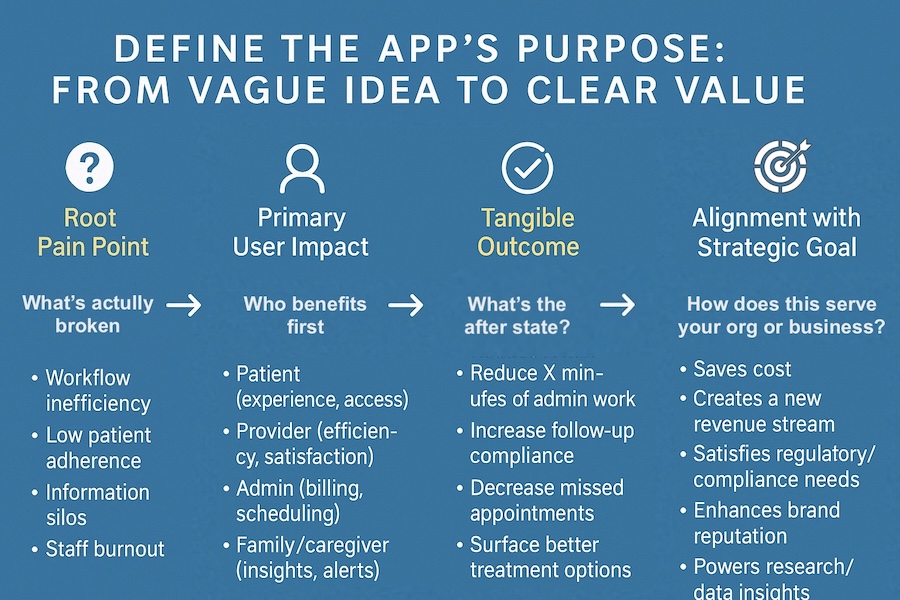
Define one pain point + one measurable win:
Pick the single problem you’re solving first, then write a sentence like: “We’ll know the app is working when…”
Examples: “no-show rate drops by X%,” “documentation time per visit drops by Y minutes,” “triage response time falls under Z,” or “after-visit instructions get acknowledged within 24 hours.”
Fast market validation checklist:
- Read competitor reviews (App Store/Google Play): what users hate is your roadmap.
- Do a quick competitor teardown: features, onboarding, pricing, and friction points.
- Validate regulatory expectations early (HIPAA, GDPR, FDA SaMD, or SOC 2 triggers).
- Confirm the workflow with real stakeholders (patients, clinicians, admins, and front-line staff).
Related: The Ultimate Guide to Building The Best mHealth Apps
Step #2: Establish compliance & privacy strategy
Define how you’ll handle PHI/PII and design your security baseline up front: encryption, access controls, audit logging, data retention, and vendor BAAs as needed. Decide what’s in scope (HIPAA, GDPR, FDA/SaMD, SOC 2, ISO 27001) and how integrations (EHR, HL7/FHIR) will be secured.
If your app influences clinical decisions or treatment, you may be building SaMD (Software as a Medical Device), which can change your documentation, testing, validation, and release discipline. Also be explicit about what data you collect. PHI is only part of the story: many health mobile products collect PII (Personally Identifiable Information) even when they don’t store clinical notes. That PII (names, contact details, identifiers, device IDs) still demands tight access control, retention rules, a clear privacy model, and breach response planning.
Treat compliance as a design constraint from day one. Default to minimum necessary access.
Security baseline you should expect from a serious healthcare build:
- Role-based access control (RBAC) + least privilege
- Strong auth (token-based auth, OAuth2/OIDC where applicable)
- Session timeouts + secure device/session handling
- Audit logs + monitoring (who accessed what and when)
- Regular vulnerability testing / penetration testing
Common misses that cause painful rework:
- No clear auditability (can’t prove access patterns)
- PHI handling scattered across services without a plan
- Insecure defaults (over-permissive roles, weak logging, leaky endpoints, and stale secrets)
- Vendor BAAs signed without checking subprocessors
Practical rule: don’t store sensitive data or credentials on the device unless the workflow truly requires it.
Also plan vendor posture (subprocessors + BAAs), retention/deletion expectations, incident readiness, and breach notification timelines.
Step #3: Build a prototype (UI/UX design & prototyping)
Create wireframes and a clickable prototype, then put the key flows in front of real users: appointment scheduling, intake, telemedicine, and messaging. This is where you learn what to delete cheaply before “medical app development” gets expensive.
What prototyping buys you (beyond “pretty screens”):
- You test the experience on the actual device, in the conditions a clinician or patient actually faces
- You A/B test the riskiest flows early
- You catch developer feasibility issues before you lock scope
- You hand stakeholders something tangible to react to
Prototype tools (pick the level that matches your stage):
- Low-fi: Balsamiq / Proto.io for quick flow validation
- Higher-fidelity: Adobe XD / InVision (or modern equivalents) for stakeholder-ready demos
Note: AI-assisted coded prototyping can be helpful, but keep PHI out of early demos and treat the prototype as disposable learning, not production code.
“It’s 10x cheaper to fix a design flaw while prototyping than during development.”
Joe Tuan, Founder and CEO, Topflight Apps
Where “coded prototyping” really helps: a clickable prototype is perfect for validating flows and usability, but a light coded prototype lets your development team test “real app” behavior earlier: navigation, data states, permissions, and edge cases, often using synthetic data and stubbed endpoints so you’re not dragging PHI into a prototype. It’s the middle ground between UX/UI and full medical mobile app development. You get enough realism to estimate effort and catch feasibility issues early, without paying for production-grade engineering too soon.
Read more about Health App Design
This is especially useful in mobile healthcare application development when the app depends on device behavior (camera, biometrics, offline mode, and location) or when “user friendly” has to hold up on an iPhone in a clinic hallway. If you’re building symptom checkers or triage flows, the prototype should also stress-test what happens when users enter messy, incomplete inputs, because they will.
Step #4: Polish design and develop (agile development & tech stack selection)
Turn validated flows into production-ready software with iterative sprints, continuous testing, deliberate integration work, and a tech stack that fits your constraints (iOS/Android, cross-platform, backend, analytics). Build integrations carefully (EHR connectivity, medical records access, dashboards, medical imaging, Laboratory Information System (LIS)) because they can dominate scope.
Design/UX rules that matter in healthcare (because interruptions are normal):
- Reduce cognitive load (clinicians don’t have time for “clever”)
- Design for interruption (autosave, drafts, clear recovery, and confirmable back navigation)
- Make the next action obvious (visual hierarchy > fancy UI)
- Match real workflows (intake → visit → discharge → follow-up)
Validation loop (keep it lightweight but real):
Run quick feedback cycles with a small group of real users (even 3-5 per audience type is useful). Tight feedback beats late “big reveal” redesigns.
And plan integration/testing early. Health apps often live inside legacy systems and EHR ecosystems, so interoperability decisions (APIs, HL7/FHIR) can reshape architecture fast.
Reality check for healthcare mobile development: incumbents rarely get to “replace the old system.” More often, you develop a custom healthcare app that has to coexist with legacy tools, electronic health records, old databases, CRMs, and even billing systems tied to health insurance. In those cases, a practical pattern is a HIPAA-compliant data hub that is the syncing link between the new app and the legacy stack.
Done right, the hub prevents double data entry for staff who still live in the EHR, while the new health application gets the data it needs for modern patient care experiences. A controlled set of APIs pushes updates from legacy systems to the new app and back again (two-way sync), with logging and access control baked in. This keeps medical application development aligned with how healthcare organizations actually modernize: gradually, without breaking day-to-day operations.
Step #5: Launch and maintain (MVP launch & user feedback loops)
Ship the MVP with analytics instrumented from day one, then run feedback loops with patients and clinicians. Plan ongoing maintenance (OS updates, security patches, performance, and dependency hygiene) and iterate on features like remote patient monitoring, wearables, telehealth, or AI-assisted documentation only after the core workflow is stable.
Pre-launch checklist (boring, but it prevents embarrassing failures):
- Final QA pass (core flows + edge cases)
- Confirm push notifications, deep links, permission prompts, and offline behavior
- Verify production data connections and access controls
- Double-check app metadata/store readiness
App launch options depend on who the users are: if you’re building a consumer product, you’ll ship to the App Store / Google Play. If it’s staff-only mobile medical software, you may distribute privately (e.g., through an internal device management approach) to control rollout and support. Either way, a soft-launch to a small cohort first gives you a buffer to catch issues early, without tanking ratings or trust on Day 1.
Once you build a medical app and it’s live, real usage drives the next iterations. If you’re trying to make a medical app stick (or help users reach outcomes faster), the analytics you already have (e.g., usage metrics from Firebase or Appsee) will show where people drop off, what features they ignore, which flows cause friction, and which segments stick. Pair that with a lightweight feedback loop: let users report issues in-app (so they don’t vent in reviews) via tools like UserVoice or UserTesting, and watch store feedback for early signals. That’s how you create a health app that keeps getting more useful after launch.
After launch: operate it like a product, not a one-time project:
- Track usage and friction with analytics (what people do vs what they say)
- Monitor crash/performance and prioritize fixes in an ongoing cadence
- Capture user feedback proactively (in-app prompts + review monitoring)
- Expect OS/platform updates to force maintenance work, and plan for it
If the product is regulated (e.g., FDA-relevant functionality), maintenance also includes disciplined change documentation and regression testing.
5 steps to create a medical app summary:
| Step | What you do | Tools and technologies |
|---|---|---|
| 1. Define your audience | Personas, workflow mapping, market research, validate the riskiest assumptions | Interviews + surveys, journey maps, competitor review mining, lightweight analytics review |
| 2. Compliance & privacy strategy | PHI/PII boundaries, regulatory posture, security baseline, vendor risk | Threat modeling, encryption, RBAC, audit logging, BAAs, pen testing, SOC 2 / ISO 27001 targets |
| 3. Prototype | Wireframes + clickable prototype, usability testing, iterate on flows, and validate feasibility with devs | Figma / Proto.io, usability sessions, A/B tests where useful, and synthetic data for early demos |
| 4. Design + develop | Agile delivery, QA, integrations, interoperability planning | iOS/Android or cross-platform, CI/CD, HL7/FHIR, EHR API strategy |
| 5. Launch + maintain | MVP release, monitoring, feedback loops, ongoing updates | App Store / private distribution, analytics, crash reporting, support + iteration cadence |
How much does it cost to create a healthcare app?
The cost of app development for healthcare depends mostly on scope, integrations, compliance, and team composition. A basic telemedicine product often lands around $260,000, and a full-cycle practice management platform can run $380,000+.
Rapid prototyping protects ROI by validating user journeys (and killing bad ideas) before you pay for full-scale medical app development in code.
If you’re using Topflight’s team to create a medical app, the minimum starting budget is $60,000 for a PoC or MVP.
Best practices and modern capabilities in healthcare app development
Best practices grounded in health care workflows
- User-centric design + usability testing on patient, provider, admin, and front-desk flows from the start
- Compliance-first (HIPAA, GDPR, FDA SaMD, and SOC 2 where applicable) + minimize PHI early (push PHI behind secure systems; start with de-identified flows when possible)
Related: HIPAA Compliant App Development: Everything You Need to Know
- Security baseline with PHI/PII handling specified up front: encryption, RBAC, access controls, audit logs, and tamper-evident trails
- Integration readiness for EHR/EMR vendors and APIs, with planning for Epic/Cerner constraints, OAuth flows, data mapping, and idempotent writes
- Interoperability via FHIR/HL7 when needed: structured exchange for referrals, labs, encounters, and orders (avoid “CSV cosplay”)
- Continuous testing, iteration, maintenance, and dependency hygiene (regression testing, monitoring, OS updates, security patch cadence)
2026+ features worth adding
- AI/ML → when you have enough clean data to automate documentation, triage, coding, or evidence-based recommendations.
- Telehealth → when remote consults and follow-ups are core to access (video + secure messaging + scheduling + audit trails).
- Wearables/IoT → when continuous monitoring matters (e.g., heart rate, blood pressure, glucose levels, and weight) and you can handle device variability.
- Interoperability (FHIR) → when you must exchange data with EHRs or clinical systems (labs/LIS, medical imaging, dashboards, and encounter records) without manual re-entry.
- AR/VR → when training, rehab, patient education, or surgical planning benefits from guided, hands-on simulations (and you can measure outcomes).
- Blockchain → when you need tamper-evident record integrity and shared trust across parties (otherwise it’s usually extra complexity).
Monetization models of a healthcare application
How healthcare apps make money depends on who pays (patients, providers, employers, payers) and what value you deliver (access, efficiency, outcomes, and cost reduction). In practice, most successful models blend more than one revenue stream.
- Subscription (B2C): monthly plans for premium features, content, coaching, or community access
- Subscription (B2B): clinics or employers pay per seat / per location
- Per-visit / usage fees: telemedicine consults, async eConsults, messaging bundles, or pay-per-session
- Licensing: sell the platform to provider orgs (often with implementation fees)
- Reimbursement / billing enablement: when the app supports billable services (e.g., RPM programs)
- Partnerships / referrals: vetted services (labs, devices, pharmacies, and DME suppliers) that fit the workflow
Avoid ad-driven monetization when the app touches sensitive patient data. It’s a fast way to lose trust and invite regulatory headaches. For teams building specifically in the pharmacy vertical, a pharmacy app development company that knows the monetization, workflow, compliance, and reimbursement realities can shorten the path from idea to live prescription management and medication fulfillment products.
How to choose a healthcare app development company
For healthcare app development, you’re buying the ability to ship a workflow product that handles sensitive data, survives EHR integrations, holds up under interruptions, and still works when real clinicians use it at 7:12 AM.
- Proven healthcare delivery experience: ask for 2-3 comparable projects (similar users, workflows, risk, and integration depth).
- Security + compliance maturity: they should already be fluent in HIPAA/GDPR basics, threat modeling, audit logs, access controls, encryption, and vendor BAAs.
- Integration capability (EHR + interoperability): look for experience with APIs, HL7/FHIR mapping, real-world Epic/Cerner constraints, and SMART on FHIR auth flows (rate limits, data normalization, sandbox quirks, and idempotent retries).
- Discovery discipline: they should run stakeholder interviews, workflow mapping, risk identification, and scope definition before sprinting into UI polish.
- UX for distinct audiences: patient, provider, admin, and front-desk flows are different products sharing one database. Your partner should design accordingly.
- Engineering quality + QA: testing strategy, release process, code review standards, and measurable quality signals (crash rate, performance, security scans, and accessibility checks).
- Open-book estimation + change control: clear assumptions, milestones, a change-order process, and what happens when scope shifts (because it will).
- Post-launch support plan: monitoring, OS update cadence, incident response, and a realistic maintenance budget. Health apps don’t “finish.”
- Data strategy: how they model and validate patient data, handle permissions, audit access, and maintain data integrity over time.
Red flags: “We’ll figure HIPAA later,” vague answers about integrations, no QA plan, or a proposal that’s 90% UI screenshots and 10% delivery plan.
In healthcare app development, picking the right custom mobile app development company shapes how the patient experience holds up under real use.
What makes healthcare app developers different from general mobile developers
Healthcare app development is its own specialty within mobile development. Hiring the wrong team is one of the most common reasons healthcare builds go over budget or stall before launch.
A healthcare app developer ships software that handles PHI without creating a HIPAA liability, integrates cleanly with Epic or Cerner, survives real clinical workflows where interruptions, edge cases, legacy system quirks, and after-hours support pages are routine, and stays defensible if FDA or OCR comes knocking.
Here’s what separates a specialist healthcare app developer from a generalist shop:
- HIPAA fluency by default. They should speak to encryption standards, BAA requirements, audit logging, and PHI minimization without prompting.
- EHR integration experience. Real FHIR/HL7 builds. Ask for specific Epic or Cerner integration examples.
- Clinical workflow knowledge. They should ask about your users’ context of use (e.g., on a tablet mid-visit vs. desktop at a nurse’s station) before writing a single line of code.
- Regulatory posture. If your app touches clinical decision-making, experienced healthcare app developers will flag FDA SaMD considerations during discovery.
- Post-launch support. Healthcare apps don’t “finish.” OS updates, security patches, dependency hygiene, and evolving compliance requirements demand a team that treats the product as an ongoing system.
When evaluating healthcare app developers, ask for 2-3 comparable case studies: matching user type (patient, provider, admin, or front-desk), similar compliance requirements, real integration work, and post-launch support records. Healthcare delivery software is its own discipline.
Develop your healthcare app with Topflight
Topflight builds web and mobile healthcare products where “it works in a demo” isn’t good enough. Our portfolio spans remote patient monitoring, telehealth, mental health, lightweight EHR-style workflows, IoT, enterprise-grade platforms, and AI-powered healthcare solutions.
Today, we can boast apps from the following healthcare specialties in our portfolio:
- Remote patient monitoring
- Telehealth
- Mental health
- Super-lightweight EHRs for clinics
- Uber for lab testing
- Fitness & wellbeing
- IoT solutions
- Enterprise-grade health applications
- AI-powered healthcare solutions
- AI/AR RPM for physiotherapy
- Uber for medical outstaffing
We typically start with rapid prototyping to validate flows, edge cases, feasibility, and effort before full development, so you don’t burn budget on the wrong build. If your app needs integrations (EHR systems via FHIR/HL7, devices, labs, and imaging) or stronger security/compliance posture, we plan that early, because in healthcare, retrofits are where timelines go to die.
If you’re ready to build a healthcare app, share your app concept and target users (patient, provider, admin, or front-desk). We’ll help you shape scope into an MVP that can launch, iterate, scale, and stay maintainable.
[This blog was originally published on March 2, 2020 but has been refreshed to keep up with more recent updates]
Related Articles:
- Physiotherapy app development guide
- Pediatrician App Development
- Mental Health Chatbots
- Guide to Creating a Pharmacy App
- Deep Learning Use Cases in Healthcare
- How to make a women health tracking app
- How to make a hospital management software
- Medication Tracker & Pill Reminder App Development Guide
- How to Collect Healthcare Data for Your Mobile Apps
- Guide to Computer Vision in Medicine
- Chatbots in Healthcare
Frequently Asked Questions
Do all healthcare apps need to be HIPAA compliant?
No, only mhealth software dealing with PHI needs to comply.
What would you suggest if you could give a single piece of advice to help me create an outstanding healthcare app?
Start with an interactive prototype and test it with real users from your target audience. Time spent on the prototype is the cheapest time in the whole project. Healthcare projects especially shouldn’t jump straight to development.
How do I make sure my application for patients remains competitive?
Use analytics tools like Mixpanel to understand how people use the app and where they hit issues. Pair that with in-app feedback prompts so users tell you about problems before they post a 1-star review in the App Store.
How long does it take to build a medical app?
There’s no such thing as an average timeline to build a medical app. Some healthcare software we’ve shipped in 6 months; other solutions took over a year, depending on scope and integration depth.
What is the main challenge when developing a healthcare mobile app?
Getting the workflow right while meeting privacy and security requirements. Most teams can build screens; fewer can design a system that handles sensitive data safely, fits real clinical operations, survives integrations, and stays defensible under audit, all without turning into a maintenance fire.
Which technologies are most commonly used in healthcare mobile app development?
Typically: native iOS/Android (or cross-platform), a secure backend (APIs + database), authentication with role-based access control, encryption and audit logging, and FHIR/HL7 to connect with EHR systems when interoperability is required.